The negative impacts of false negatives
The negative impacts of false negatives
What Is a False Negative?
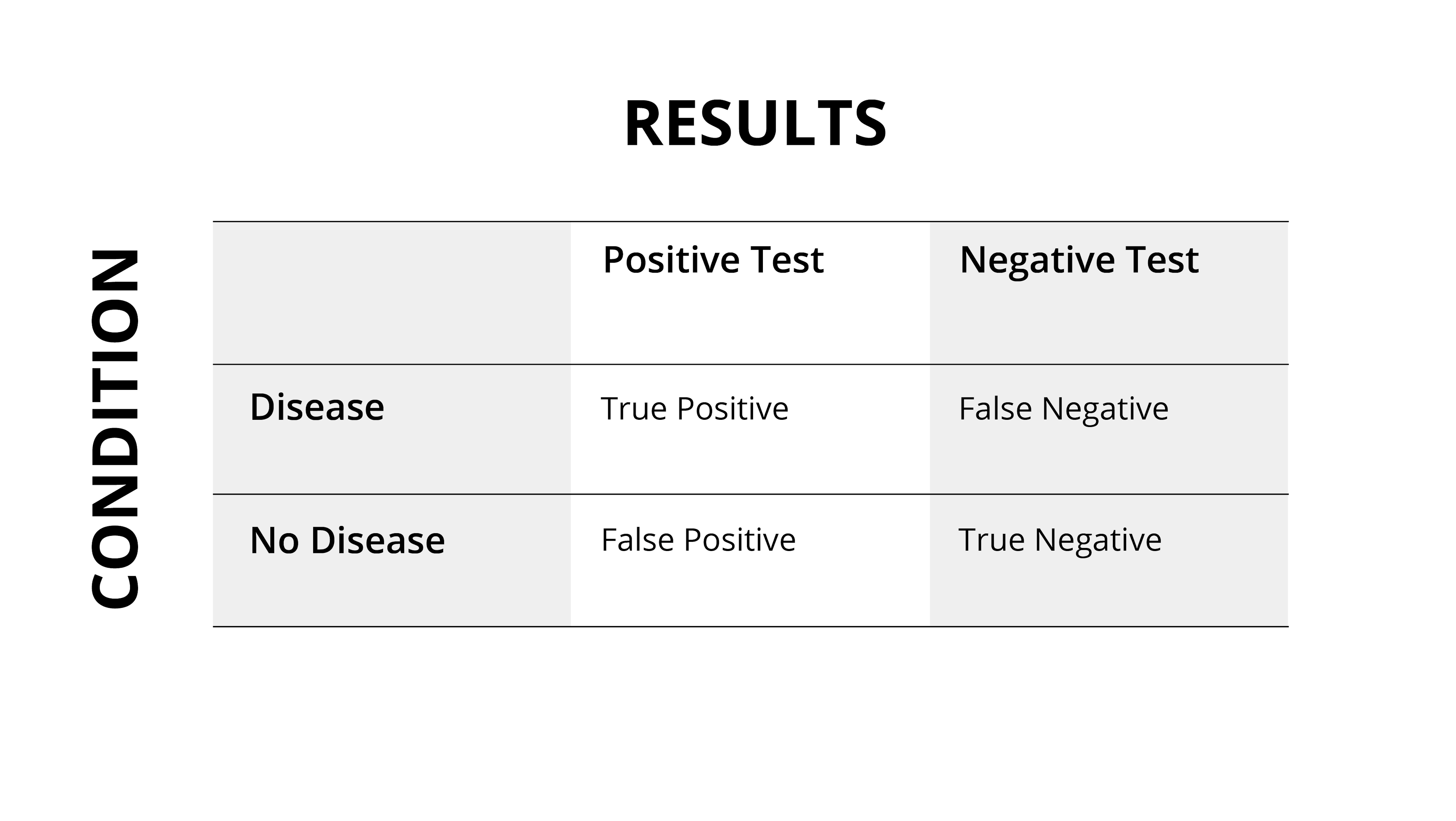
Testing for conditions and diseases can be lifesaving. For example, routine screenings for cancer can help doctors catch a problem early and provide patients with potentially life saving care. Additionally, testing for diseases which spread between people, from sexually transmitted diseases to COVID-19, is crucial for public health. When a person is made aware that they have a transmittable disease, they can take precautions to make sure it does not spread to others.
The issue is that very few tests and screenings are 100% accurate. A false negative is a test result telling someone that they do not have a disease when they actually do. False negatives can occur for a variety of reasons. Sometimes laboratories make errors. Sometimes, in the case of COVID-19, if a person’s viral load is low, not every test can identify the virus in a person’s system.
Understanding Tests’ False Negative Rates
To understand a test’s accuracy, you can use what is known as a false negative rate or FNR. To calculate a test’s FNR, take the number of false negatives divided by the total number of false negatives and true positives. A true positive refers to a situation when a disease or condition is correctly identified by a test. Here is the formula for calculating a test’s false negative rate:
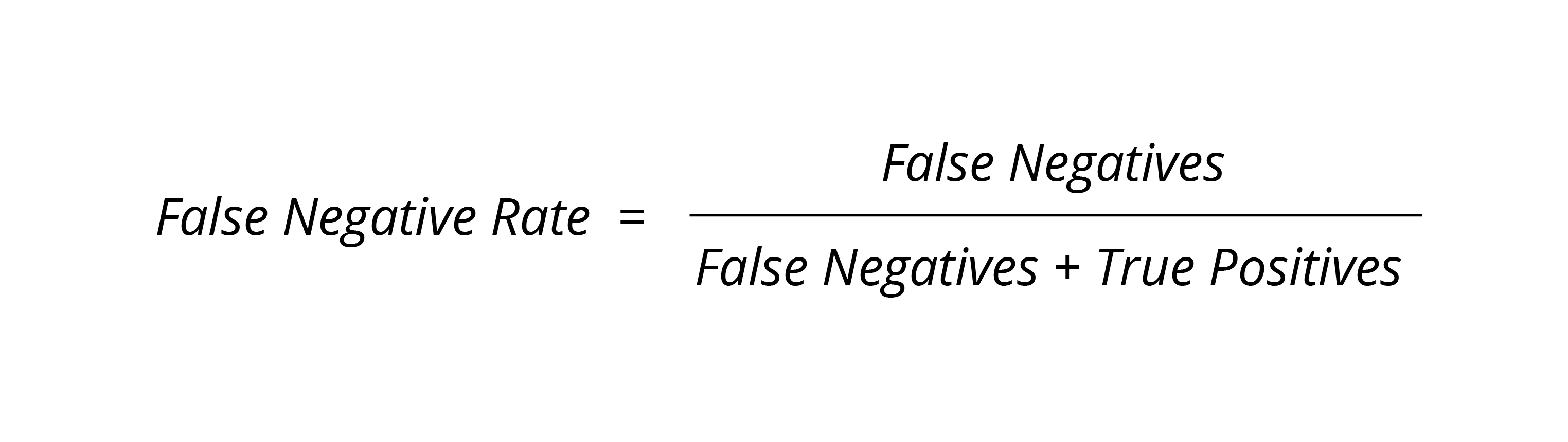
Testing has been in the spotlight over the past year-and-a-half because of the COVID-19 pandemic. When it comes to COVID-19 testing, PCR tests are considered the gold standard. In a 2021 study, PCR tests correctly identified 99.95% of all participants tested.1 We will discuss additional testing methods, including their strengths and shortcomings, in upcoming Swabology posts.
The Impact of False Negatives
To understand how false negatives impact public health, let’s think like an epidemiologist. The transmission rate of diseases are affected by the transmissibility of the disease itself, immunity in a population (either through infection or vaccination), and social behavior, among other things. In a scenario where there is a highly transmissible virus and the available testing has a significant false negative rate, it’s clear to see how this could increase the expected number of new infections from an infected individual since individuals would incorrectly believe they do not have a disease, when in reality they could be unknowingly spreading it. The impact of these false negatives could be massive. With highly infectious diseases like COVID-19, misclassifying people with infections as uninfected can lead to high transmission, especially when treatments and vaccines are limited.
False negatives can also have other detrimental impacts. For example, a recent breast cancer study showed that patients whose tumors were not detected by tests did not receive timely care and had higher morbidity and mortality than those whose tumors were identified early by tests.2Negative tests also bring about financial consequences. Medical expenses for treating diseases at later stages tend to be far higher than expenses for treatment when a disease is diagnosed early.3 Given the many consequences of false negatives, it is important to try to reduce them.
Why False Negatives Occur and How to Prevent Them
In the context of virus detection and disease diagnosis, multiple factors can cause false negative results.
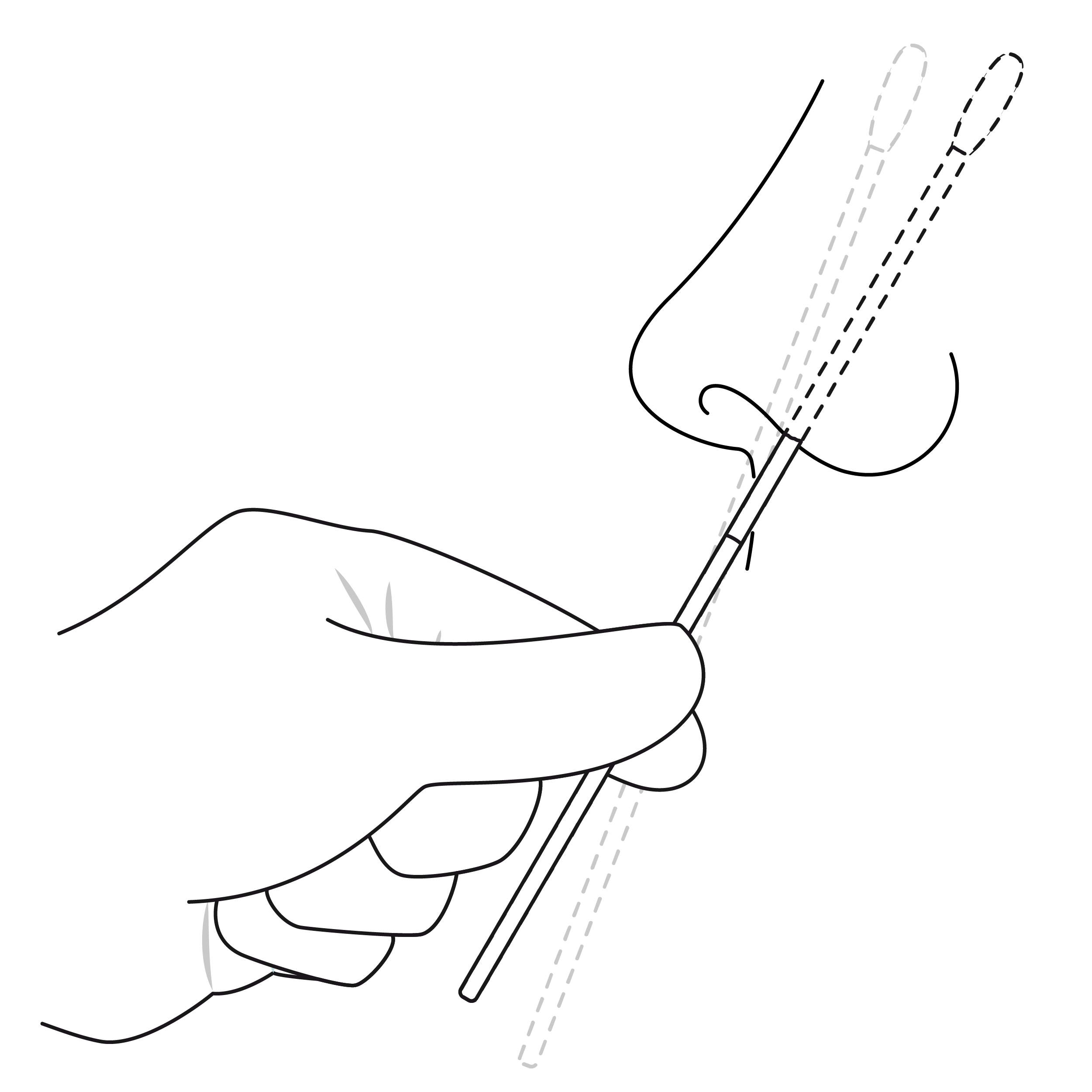
- Sampling location can make a difference when it comes to FNR. For example, a recent study of COVID-19 testing found that nasopharyngeal (nasal) samples are much less likely to result in false negative results than oropharyngeal (oral) ones.4
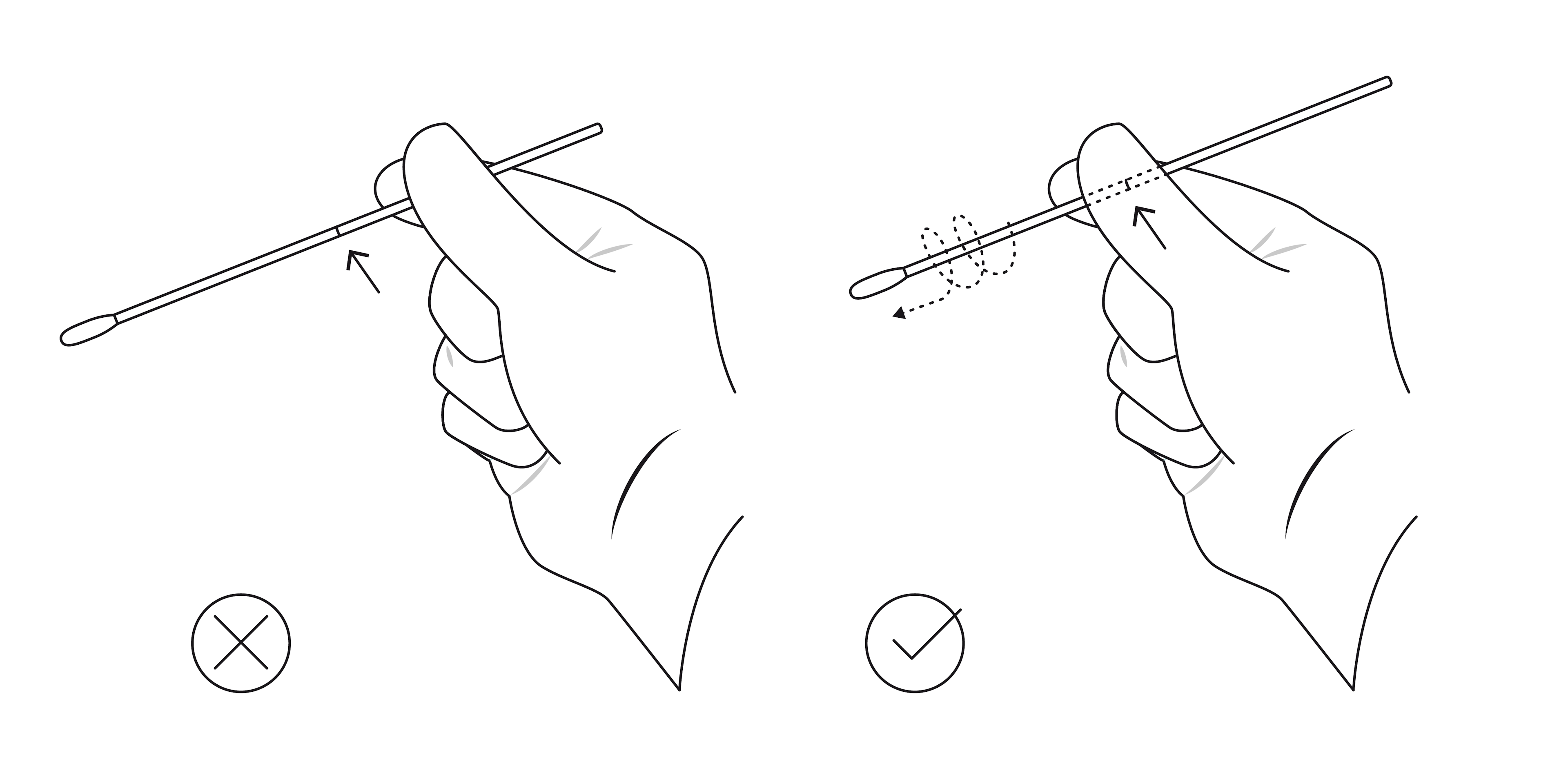
- Training for those performing tests is also vital. For example, if a nasal swab is not inserted or rotated correctly, test performance can be impacted.5
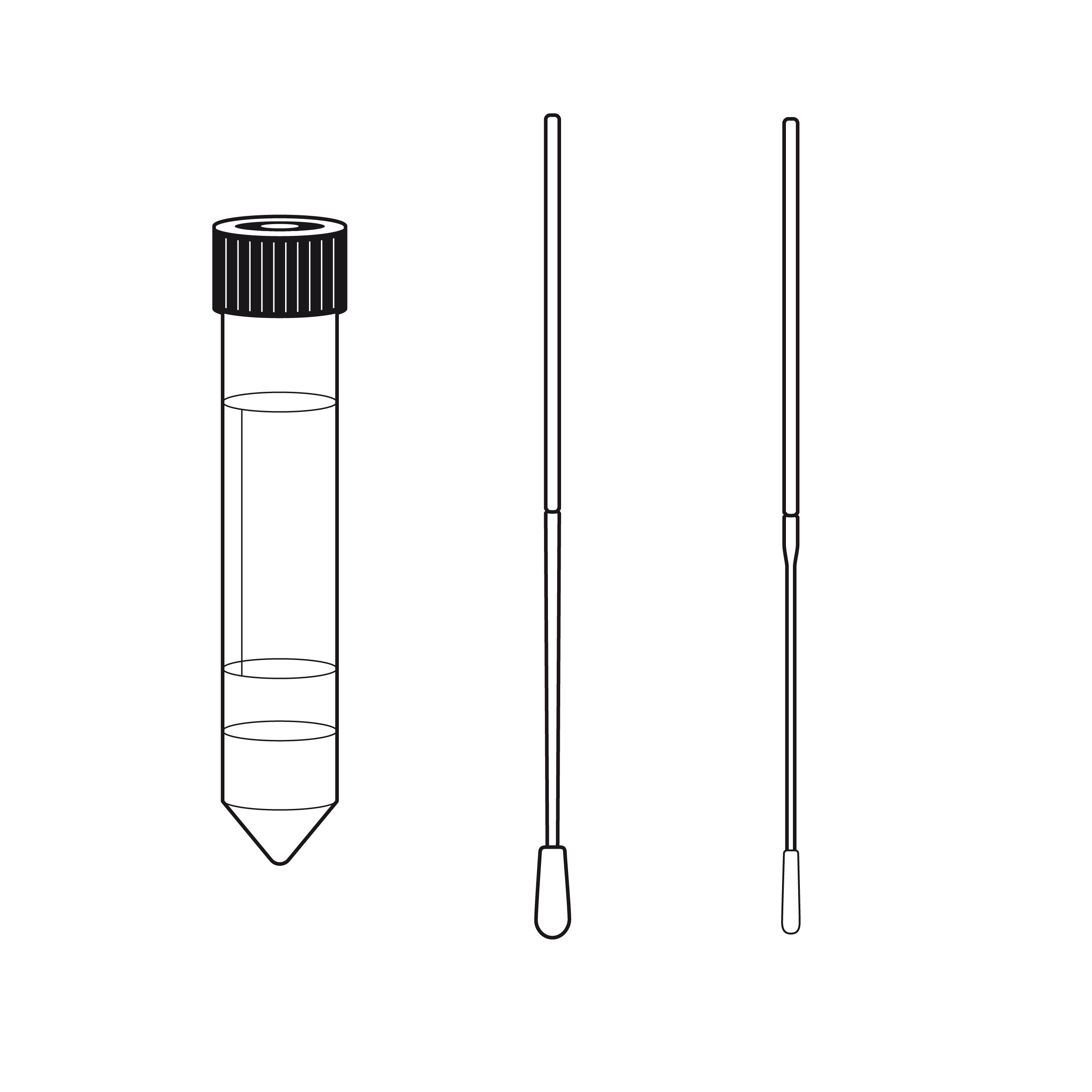
- Materials used for collection can also contribute to or decrease false negatives. Technologically advanced swabs, like Instaswab, can impact how effectively samples are transferred from a patient to a laboratory for testing.6 For example, a study showed that when testing for HPV using vaginal self-samples, flocked swabs performed better than cotton swabs.7
In another example, InstaSwab outperformed polyester and flocked swabs_in an in vitro qPCR study, detecting virus at extremely low viral loads and returning an amplification when the others could not.
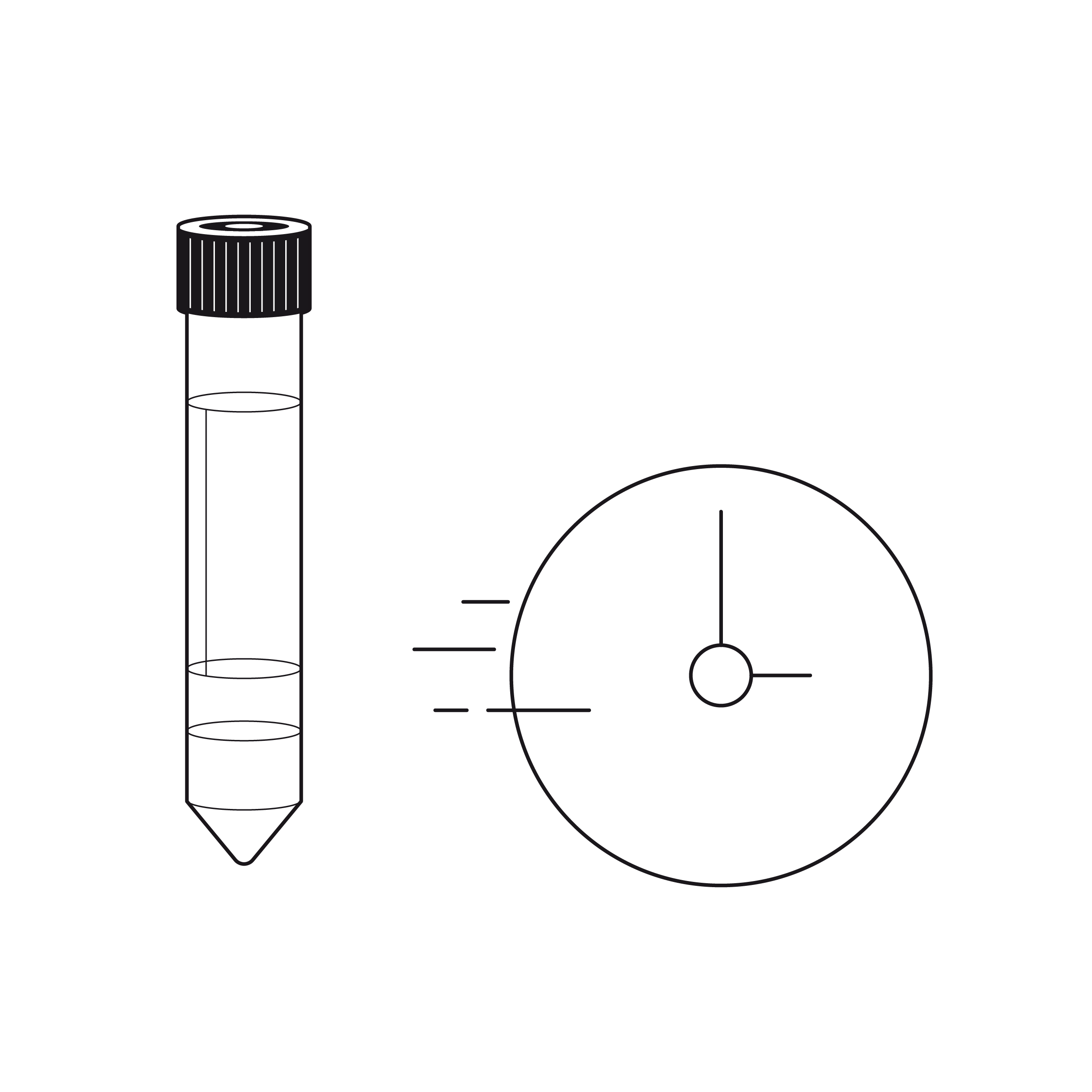
- Timing is also a factor when it comes to false negatives. For instance, false negatives in HIV testing mostly occur during the first few weeks after infection, but they rarely happen after that period.8 For this reason, consecutive tests at slightly different periods in time can help prevent false negatives.
- Genetic variation of viruses is another contributing factor. Viruses mutate over time. If the part of the viruses’ genome that is assessed by tests has a mutation, tests may no longer recognize the virus, which can cause false negatives. However, molecular tests designed to detect multiple genetic targets tend to be less impacted by virus mutations than tests designed to detect one genetic target.9
Looking Ahead
A number of factors can help prevent false negatives, from more advanced materials for sample collection to better training for medical professionals. It is also important to make tests for all sorts of conditions more accessible and affordable. Preventing false negatives and their consequences can lead to improved health for individuals as well as communities.
Bibliography
- Kanji JN, Zelyas N, MacDonald C, et al. False negative rate of COVID-19 PCR testing: a discordant testing analysis. Virol J. 2021;18(1):13. doi:10.1186/s12985-021-01489-0
- Kaufman PA, Bloom KJ, Burris H, et al. Assessing the discordance rate between local and central HER2 testing in women with locally determined HER2-negative breast cancer. Cancer. 2014;120(17):2657-2664. doi:10.1002/cncr.28710
- Petticrew M, Sowden A, Lister-Sharp D. FALSE-NEGATIVE RESULTS IN SCREENING PROGRAMS: Medical, Psychological, and Other Implications. Int J Technol Assess Health Care. 2001;17(2).
- Wang X, Tan L, Wang X, et al. Comparison of nasopharyngeal and oropharyngeal swabs for SARS-CoV-2 detection in 353 patients received tests with both specimens simultaneously. Int J Infect Dis. 2020;94:107-109. doi:10.1016/j.ijid.2020.04.023
- Bahreini F, Najafi R, Amini R, Khazaei S, Bashirian S. Reducing False Negative PCR Test for COVID-19. Int J MCH AIDS. 2020;9(3):408-410. doi:10.21106/ijma.421
- Zasada AA, Zacharczuk K, Woźnica K, Główka M, Ziółkowski R, Malinowska E. The influence of a swab type on the results of point-of-care tests. AMB Express. 2020;10(1):46. doi:10.1186/s13568-020-00978-9
- Viviano M, Willame A, Cohen M, et al. A comparison of cotton and flocked swabs for vaginal self-sample collection. Int J Womens Health. 2018;10:229-236. doi:10.2147/IJWH.S157897
- Pebody R. False negative results on HIV tests. https://www.aidsmap.com/about-hiv/false-negative-results-hiv-tests. Published June 2021. Accessed June 30, 2021.
- FDA. Genetic Variants of SARS-CoV-2 May Lead to False Negative Results with Molecular Tests for Detection of SARS-CoV-2 – Letter to Clinical Laboratory Staff and Health Care Providers. https://www.fda.gov/medical-devices/letters-health-care-providers/genetic-variants-sars-cov-2-may-lead-false-negative-results-molecular-tests-detection-sars-cov-2. Published 2021. Accessed June 30, 2021.